Blueprint: Medical Documentation Automation & Data Governance
Target Industry: Healthcare Organizations, Hospitals, Clinics, Healthcare Insurance
1. Blueprint: Medical Documentation Automation & Data Governance
Physicians today face a growing documentation burden, spending up to 2–3 hours per day on administrative tasks like writing clinical notes, discharge summaries, and updating electronic health records. This not only contributes to physician burnout but also limits the time they can devote to patient care.
We propose an intelligent medical documentation automation system that transcribes physician-patient conversations in real time and generates structured clinical outputs, including SOAP notes, discharge summaries, ICD-10 codes, and care plans. Powered by AI and integrated seamlessly into existing health infrastructure, this solution significantly reduces redundant manual work and empowers clinicians to focus on their medical expertise and patient relationships.
2. The Problem We’re Solving
Modern healthcare professionals are overburdened with documentation tasks that detract from the core value of clinical practice: patient care. Manual note-taking is time-consuming, error-prone, and often inconsistent across departments and providers. The growing demand for accuracy in medical coding and regulatory compliance only adds to this load.
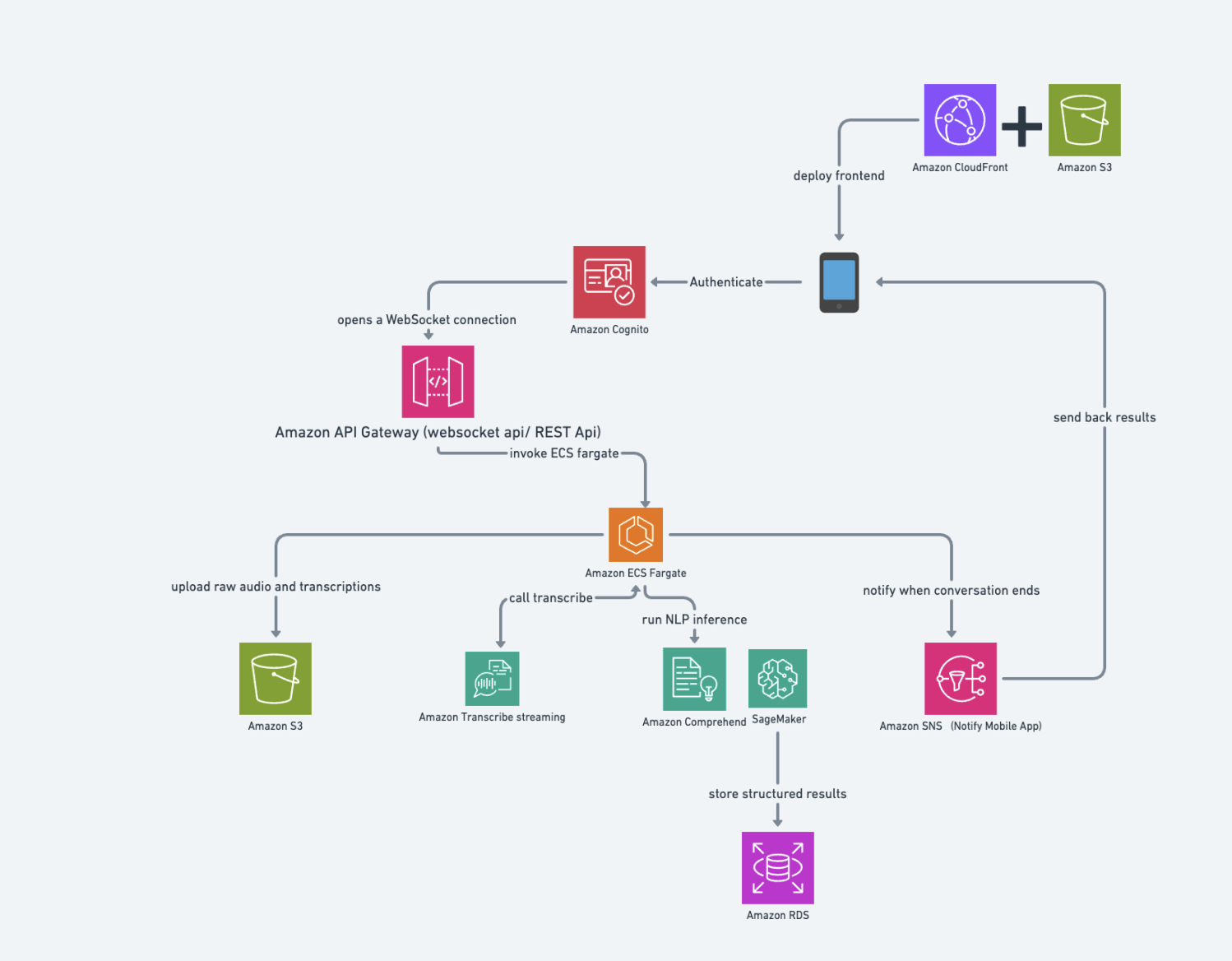
3. Architecture Overview
Our architecture (as illustrated above) enables real-time capture, transcription, and transformation of clinical dialogue into structured data using secure and scalable AWS services. It supports both live interactions and post-hoc uploads while ensuring robust access control, performance, and interoperability.
Key Workflow:
- Real-Time Audio Capture
- The system opens a secure WebSocket connection with a frontend (mobile or web) deployed via Amazon CloudFront and S3.
- Physicians can authenticate via Amazon Cognito and initiate recording through the app.
- Transcription Pipeline
- The raw audio stream is sent through Amazon API Gateway and passed to Amazon ECS Fargate, where it calls Amazon Transcribe Streaming to convert speech to text in real time.
- AI-Powered Clinical Inference
- Transcribed text is sent to Amazon Comprehend Medical or Bedrock-hosted models to extract medical entities, summarize notes, and generate structured outputs such as:
- SOAP Notes
- ICD-10 Medical Codes
- Discharge Summaries
- Personalized Care Plans
- Transcribed text is sent to Amazon Comprehend Medical or Bedrock-hosted models to extract medical entities, summarize notes, and generate structured outputs such as:
- Structured Data Storage
- Cleaned and enriched records are stored in Amazon RDS, providing easy access for downstream EHR integration or compliance tracking.
- Notification & Delivery
- On session completion, Amazon SNS notifies the physician or administrative staff, and the finalized documentation is returned to the frontend.
- Data Upload Option
- For asynchronous workflows, clinicians may also upload raw audio directly to S3, triggering the same processing pipeline.
EHR Integration & Data Management
To maximize utility and continuity of care, the automated documentation pipeline is designed for seamless integration with existing Electronic Health Record (EHR) systems. Structured outputs, such as clinical notes, medical codes, and care plans, are formatted to align with standard HL7/FHIR schemas, ensuring compatibility with popular EHR platforms like Epic, Cerner, and Meditech.
This integration supports both real-time and batch ingestion modes:
- Real-Time Sync: Documentation is automatically pushed to the appropriate patient record as soon as a session ends.
- Batch Mode: Admins can review, approve, and bulk-upload finalized records on a scheduled basis.
In addition to write-backs, the system supports EHR data enrichment by intelligently referencing historical patient information (medications, diagnoses, lab results) to contextualize new entries and flag potential gaps in care plans.
Structured data is securely stored in Amazon RDS for longitudinal analysis, predictive care, and clinical research ensuring the automation layer integrates seamlessly with existing clinical workflows rather than operating in isolation.
4. Strategic Benefits to Healthcare Providers
By automating medical documentation through AI, hospitals and health systems gain:
- Time Savings
Physicians reclaim hours each day, reducing after-hours work and freeing time for clinical care and research. - Reduced Burnout, Improved Retention
By minimizing documentation fatigue, organizations can better retain skilled clinicians and support a healthier workplace. - Consistent, Structured Records
Standardized outputs (ICD-10, care plans, notes) improve interoperability and reduce discrepancies across departments. - Increased Billing Accuracy
Automatic coding ensures better documentation of patient visits, maximizing reimbursements and compliance. - Scalable Integration
The architecture supports easy EHR integration, is cloud-native, and built to scale with future AI enhancements (e.g., summarization, risk scoring).
5. Governance, Privacy & Compliance
The solution is designed with a healthcare-first approach to data governance and security:
- Role-based access via Amazon Cognito
- Auditability and logging
- Encrypted data in transit and at rest
- HIPAA-ready services across the AWS stack
- Configurable retention and export policies
6. Looking Ahead: Towards Clinical Workflow Intelligence
This blueprint lays the foundation for a future-ready healthcare environment, where AI works quietly in the background, handling routine documentation tasks, alerting staff when needed, and ensuring structured data flows seamlessly between stakeholders.
By turning physician-patient conversations into actionable insights, healthcare institutions can boost efficiency, reduce burnout, and elevate the quality of care, all without disrupting the natural flow of clinical practice.
